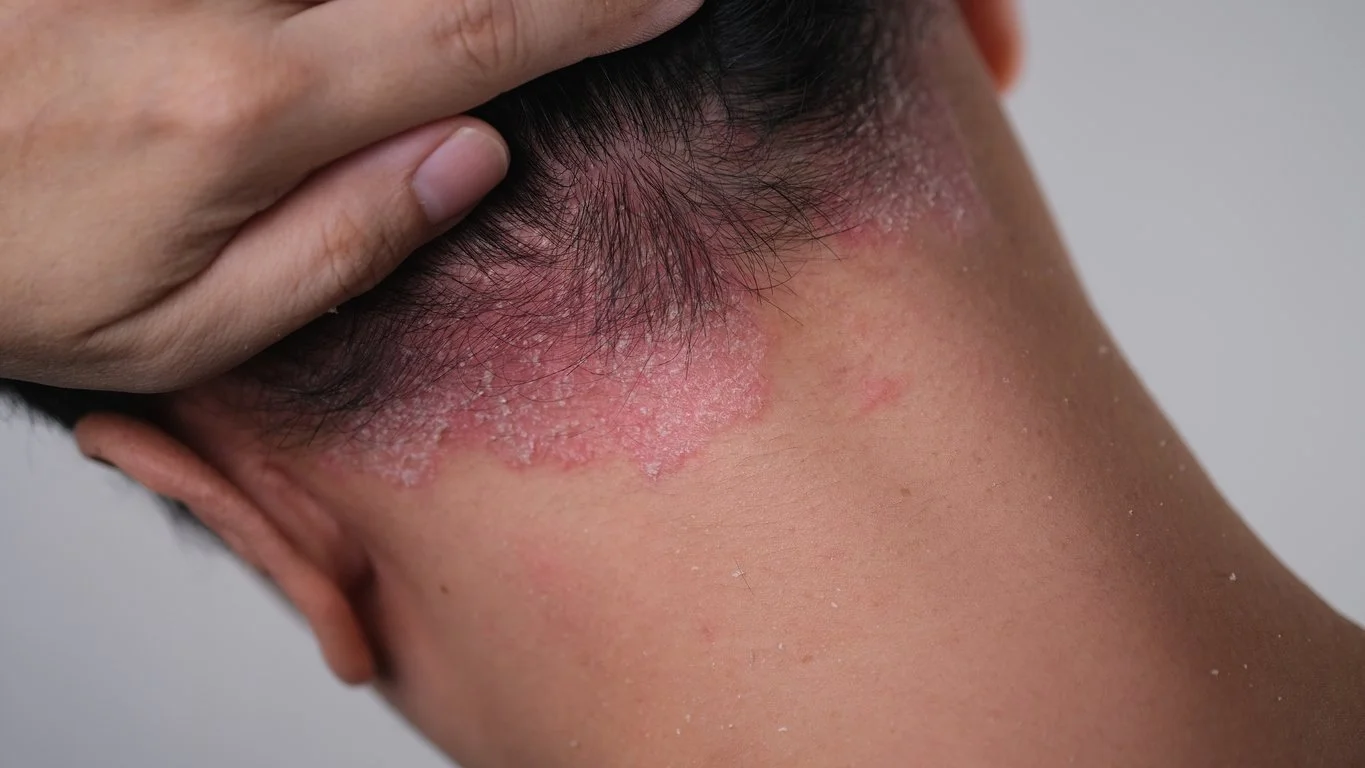
The Gut-Skin Connection in Psoriasis: How Gut Health May Influence Symptoms
Psoriasis is often approached as a condition that primarily affects the skin. However, many people living with psoriasis notice that their symptoms seem to be influenced by more than just what is happening on the surface.
Flares may come and go without a clear pattern, and some individuals begin to notice links with factors such as stress, diet, alcohol, or even digestive symptoms. This has led to growing interest in whether there may be underlying processes contributing to psoriasis beyond the skin itself.
Increasingly, research is exploring psoriasis as a systemic inflammatory condition, with potential links to gut health, the immune system and the microbiome.
Image: wisely at istockphoto.com
Psoriasis as a systemic inflammatory condition
Psoriasis is considered an immune-mediated inflammatory condition. It involves complex interactions between the immune system and skin cells, leading to the characteristic rapid turnover of skin and plaque formation.
However, inflammation in psoriasis is not limited to the skin. Studies have shown that psoriasis is associated with wider systemic processes, including:
chronic low-grade inflammation
changes in immune system regulation
associations with metabolic health
links with other inflammatory conditions
This broader perspective helps explain why some people experience symptoms or conditions alongside psoriasis, and why lifestyle factors may influence flare patterns.
Understanding the gut-skin connection in psoriasis
The gut–immune connection
A key area of interest is the relationship between the gut and the immune system.
A significant proportion of the immune system is located in and around the gastrointestinal tract. The gut plays an important role in:
regulating immune responses
maintaining tolerance to foods and microbes
acting as a barrier between the external environment and the body
When gut function is disrupted, it may influence immune activity in ways that could be relevant for inflammatory conditions.
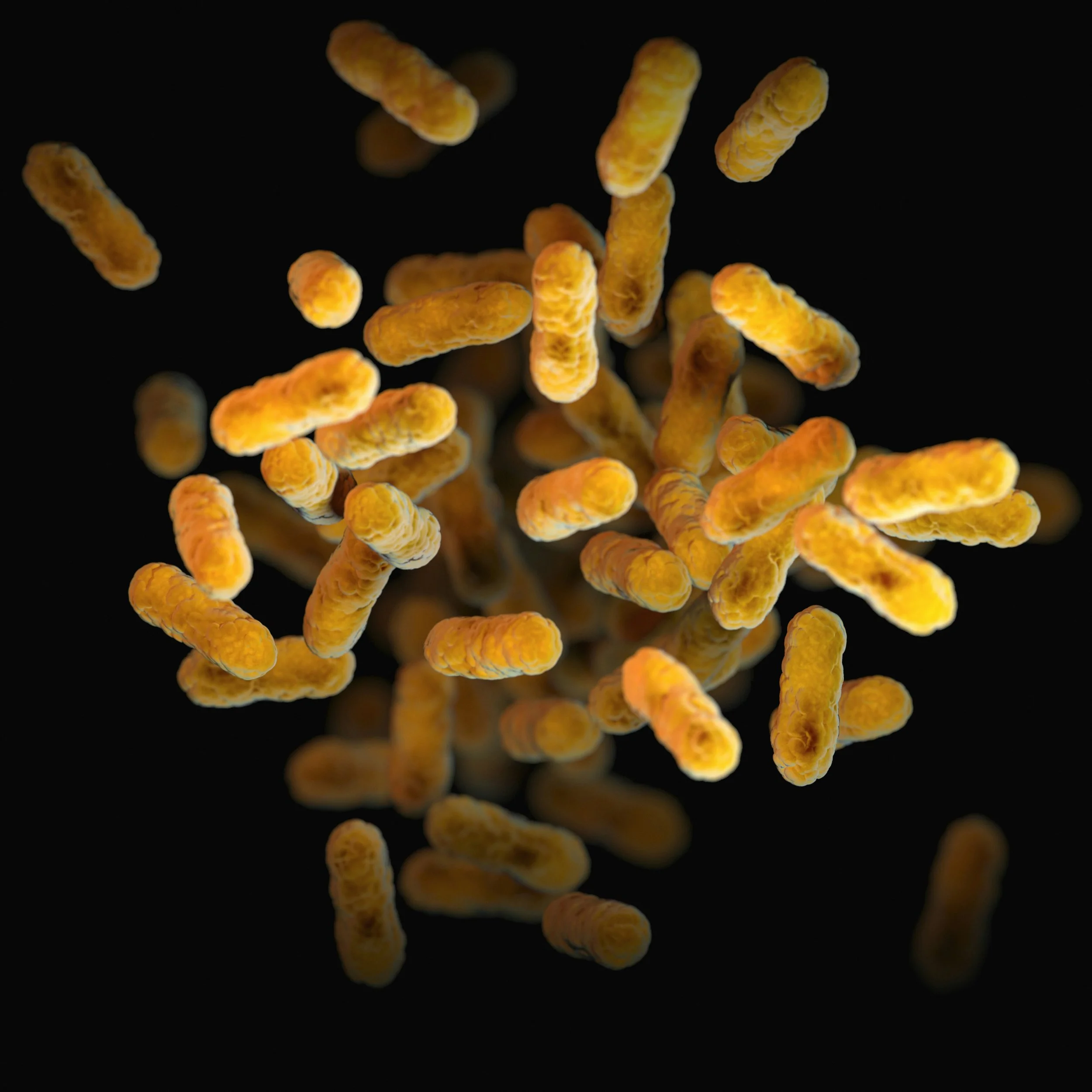
The role of the gut microbiome in psoriasis
The gut microbiome — the community of microorganisms living in the digestive tract — has been increasingly studied in relation to immune and inflammatory conditions, including psoriasis.
Some research has identified differences in the composition and diversity of the gut microbiome in individuals with psoriasis compared to healthy controls.
While this area is still developing, it is thought that changes in the microbiome may influence:
inflammatory signalling pathways
immune system activity
the balance between pro- and anti-inflammatory responses
These mechanisms may help explain, in part, how gut health could play a role in conditions that affect the skin.
Gut barrier function and inflammation
Another concept often discussed in relation to the gut–skin connection and psoriasis is gut barrier function.
The lining of the gut acts as a selective barrier, allowing nutrients to be absorbed while limiting the passage of potentially harmful substances such as toxins, microbes and undigested food particles.
If this barrier becomes more permeable (sometimes referred to as increased intestinal permeability), it may allow substances to pass into the bloodstream that can stimulate immune responses and contribute to systemic inflammation.
This is one of the proposed mechanisms by which gut health could influence inflammatory conditions, although it is important to note that research in this area is ongoing.
Why digestive symptoms may be relevant in psoriasis
In clinical practice, many people with psoriasis also report digestive symptoms such as:
bloating
abdominal discomfort
IBS-type symptoms
reflux
food sensitivities
This does not necessarily mean that digestive issues are the cause of psoriasis. However, it may suggest that, for some individuals, there is an overlap worth exploring.
Looking at gut health in these cases can sometimes help identify patterns or contributing factors that may otherwise be overlooked.
Photo by Foad Roshan on Unsplash
What this means in practice
Understanding the potential gut–skin connection does not mean that there is a single dietary approach that works for everyone with psoriasis.
Instead, it highlights the importance of a personalised approach, which may involve exploring:
dietary patterns and potential triggers
gut health and digestive function
overall inflammatory load
lifestyle factors such as stress and sleep
For some individuals, addressing these areas may help to support overall health and potentially influence how their psoriasis presents or fluctuates over time.
A balanced perspective
It is important to emphasise that nutritional therapy and lifestyle approaches are not a replacement for medical care.
Psoriasis is a complex condition, and medical treatment is often an important part of management. Nutritional therapy can be used alongside medical care as a complementary approach, helping to explore potential contributing factors and support overall health.
A brief note from my clinical perspective
In practice, I often see an overlap between psoriasis and digestive symptoms such as bloating, IBS or food sensitivities.
This has shaped my interest in the gut–skin connection and the role that nutrition and lifestyle factors may play in supporting individuals with psoriasis.
It is one of the reasons I take a personalised approach, as these patterns can look different for each individual.
Considering a more personalised approach
If you are living with psoriasis and feel that factors such as diet, digestion or lifestyle may be influencing your symptoms, a personalised approach can help explore this in more detail. If you would like to make some simple first steps, you can read my blog on common foods that may be problematic when supporting psoriasis here.
You can learn more about my approach to supporting psoriasis through personalised nutritional therapy here.