The Gut-Liver-Skin Axis: Understanding the Internal Landscape of Psoriasis
When most people think about psoriasis, they think about the skin. The plaques, the scales, the itch, the self-consciousness. And understandably so, it's the skin where psoriasis makes itself visible, and it's the skin where many treatments are directed.
But psoriasis doesn't begin at the skin. For many people, it begins much deeper — in the gut, in the liver, in the immune landscape that connects them. Understanding this internal geography is one of the most important shifts a person with psoriasis can make. Because when you understand where the fire is actually coming from, you can start to think about what might genuinely put it out.
This blog tells the story of the gut-liver-skin axis, a complex, interconnected system that research is increasingly recognising as central to the origins and persistence of psoriatic disease.
The gut - where the story often begins
Your gastrointestinal tract is far more than a tube that processes food. It is the body's largest immune organ, housing approximately 70% of your immune cells in the tissue lining the gut wall. It is also home to your microbiome — the vast community of bacteria, fungi, viruses and other microorganisms that live in your digestive system and play a profound role in regulating inflammation, immunity and overall health.
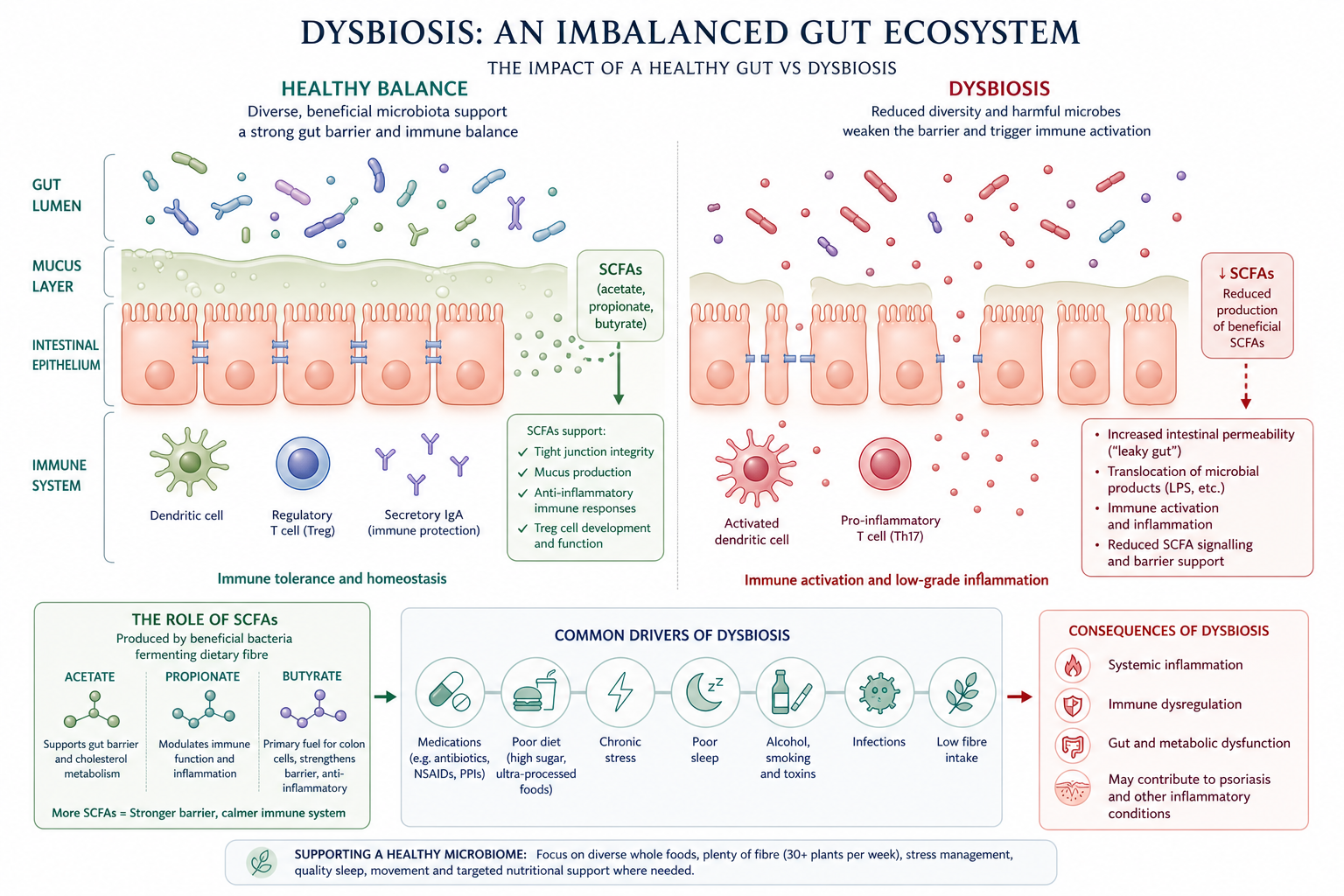
In people with psoriasis, the gut microbiome frequently looks different from that of people without psoriasis. Research consistently finds reduced microbial diversity and altered populations of key bacterial species — with some pro-inflammatory bacteria appearing in greater numbers, and beneficial, anti-inflammatory species in decline. This isn't simply a coincidence. The gut microbiome is one of the primary modulators of the immune system, and shifts in its composition, often termed ‘dysbiosis’, can tip the immune system from a balanced, regulated state (involving regulatory T cells (Treg) into a chronically pro-inflammatory one (with involvement of inflammatory ‘self-attack’ T helper cells, e.g., Th17).
One of the key ways this happens is through the production of short-chain fatty acids (SCFAs). SCFAs are chemical compounds produced when beneficial gut bacteria ferment dietary fibre consumed as part of a healthy diet. SCFAs, particularly butyrate, play a critical role in maintaining the integrity of the gut lining and regulating immune responses. When SCFA production declines, as it does when beneficial bacteria are depleted, the gut's protective barrier begins to weaken.
The leaky gut connection
The gut wall is designed to be selectively permeable, allowing nutrients, water and beneficial compounds through into the bloodstream, while keeping larger molecules, bacteria and toxins contained within the gut. This selective permeability depends on a system of tight junctions, which are essentially molecular ‘gatekeepers’ between the cells of the gut lining.
When the gut microbiome is disrupted, these tight junctions can loosen. The gut lining becomes more permeable than it should be, a state that is sometimes referred to as increased intestinal permeability, or colloquially, leaky gut. When this happens, bacterial components (such as lipopolysaccharide LPS), undigested food particles, toxins, and other molecules that should remain inside the gut can pass through into the bloodstream.
The immune system — always on alert for foreign invaders — responds to these escaped molecules with inflammation. And this is where the connection to psoriasis becomes clinically significant. Research has found that bacterial markers (e.g., LPS) and gut-derived molecules are present in the blood of psoriasis patients at higher levels than in non-psoriasis ‘healthy’ individuals, suggesting that what is happening in the gut is directly feeding the systemic inflammatory environment that drives psoriatic skin lesions.
A 2024 study using a rigorous research methodology established a causal, not merely associative, relationship between gut microbiota composition and psoriasis risk. The direction of influence runs both ways: gut dysbiosis contributes to psoriatic inflammation, and the systemic inflammation of psoriasis can in turn affect the gut. It is a cycle that, once established, tends to self-perpetuate.
Enter the liver - the body's overlooked filter
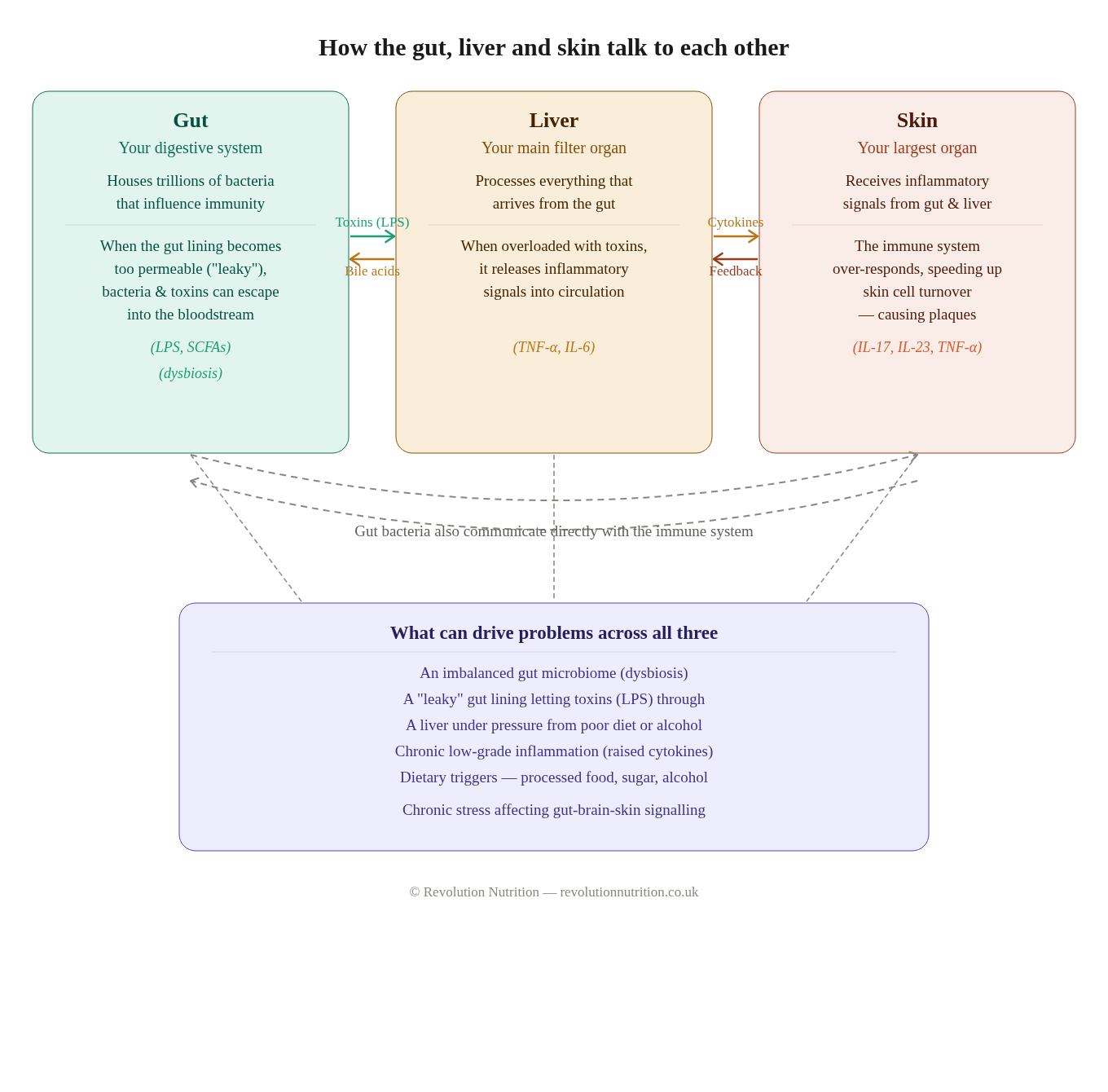
Between the gut and the systemic circulation sits one of the body's most important organs: the liver. Everything that is absorbed from the gut — nutrients, metabolites, and, in the case of a leaky gut, bacterial components and toxins — travels first to the liver via the hepatic portal vein before entering the general circulation.
The liver's job is formidable. It processes this incoming traffic, neutralising harmful substances through its detoxification pathways, producing bile acids that support digestion and gut health, regulating immune signalling, and filtering the blood before it reaches the rest of the body.
In people with psoriasis, the liver is under particular pressure. The systemic inflammatory cytokines — the pro-inflammatory signalling molecules such as TNF-α, IL-17 and IL-23 that are chronically elevated in psoriasis — don't just affect the skin. They reach the liver, where they can contribute to inflammation, impaired detoxification, and metabolic stress. Research has established that people with psoriasis have a significantly elevated risk of non-alcoholic fatty liver disease and other liver conditions, and that this connection is driven by shared inflammatory pathways, not simply lifestyle factors.
The liver also produces bile acids, and this is where things get particularly interesting for psoriasis. Bile acids are not merely digestive agents. They have direct antimicrobial properties, help regulate the gut microbiome, and play a role in controlling inflammatory signalling. When liver function is compromised and bile acid production or flow is impaired, the gut microbiome loses one of its key regulators, potentially contributing to further imbalance and inflammation.
Research into the bile acid-psoriasis connection has produced striking findings. Psoriasis patients show significant alterations in bile acid composition, and studies exploring bile acid supplementation in psoriasis have found meaningful reductions in symptoms, a finding that points directly to the gut-liver-skin axis as a clinically relevant target.
How gut metabolites reach the skin
The connection between gut and skin is not simply a matter of inflammation travelling through the bloodstream, though that is part of it. The gut microbiome produces a vast array of metabolites (chemical compounds that influence physiology throughout the body) and several of these have direct relevance to psoriasis.
Tryptophan metabolism is one particularly important example. Tryptophan is an amino acid found in food that the gut microbiome helps to process into various metabolites. In a healthy gut, this process produces indole compounds that activate a receptor called the Aryl hydrocarbon receptor (AhR), which plays a key anti-inflammatory role in both the gut lining and the skin. In people with psoriasis, research has found that protective tryptophan metabolites are significantly reduced, while pro-inflammatory metabolites from a competing pathway are elevated. This pattern may contribute to the chronic inflammatory cycle driving psoriatic disease.
Short-chain fatty acids also travel beyond the gut. Butyrate and other SCFAs have systemic effects, including direct anti-inflammatory actions in skin tissue. When SCFA production is low, the skin loses some of this protective influence.
And then there is the immune axis itself. The gut microbiome profoundly shapes the balance between pro-inflammatory Th17 cells and regulatory Treg cells, the very immune balance that is disrupted in psoriasis. Specific bacterial metabolites, including secondary bile acids produced from the liver's primary bile acids by gut bacteria, directly regulate this Th17/Treg balance. When the gut-liver axis is dysfunctional, this immune balance is harder to maintain.
Why this matters for how psoriasis is managed
The conventional approach to psoriasis management focuses on the skin, topical treatments, phototherapy, and increasingly sophisticated biologics that target specific inflammatory pathways. These can be highly effective at managing symptoms, and for many people they are an important part of living with psoriasis.
But they don't address the gut. They don't address the liver. They don't restore the microbiome, repair the gut barrier, or correct the metabolic and immune dysregulation that originates upstream of the skin.
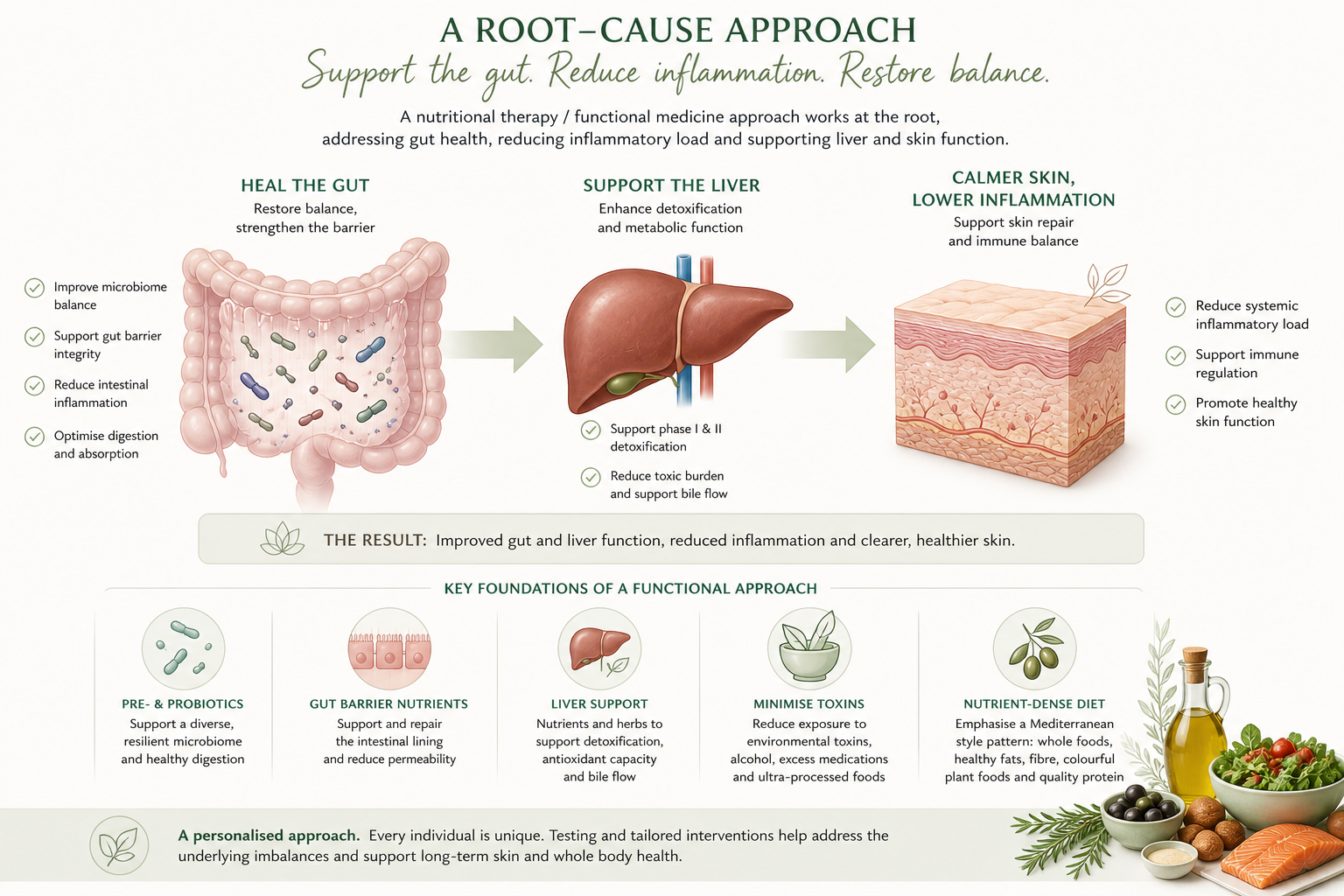
This is why a nutritional and functional medicine approach to psoriasis looks so different. Rather than beginning at the skin, it often begins at the gut, investigating the state of the microbiome, the integrity of the gut barrier, the status of liver detoxification, and the inflammatory load coming from within the digestive system. It then works systematically to restore the upstream environment that the skin ultimately reflects.
This might include restoring microbial diversity through dietary change, targeted prebiotic and probiotic support, and the removal of factors that are damaging the microbiome. It might include supporting the gut lining through specific nutrients that help repair tight junctions and reduce intestinal permeability. It might include supporting liver detoxification pathways through nutrition — ensuring the liver has the micronutrients it needs to process the inflammatory burden being passed up from the gut. And it will almost always include reducing the overall dietary and lifestyle inflammatory load that makes all of these systems harder to maintain.
A different starting point
Psoriasis is not just a skin disease. It is a systemic condition that for many people begins in the complex internal landscape of the gut-liver-skin axis. Understanding that landscape, and working to restore it, is one of the most powerful things a person with psoriasis can do alongside conventional care.
The skin, so often the focus of attention, is frequently the last place the story ends and rarely where it begins.
Kirsty Groves is a registered nutritional therapist and founder of Revolution Nutrition, specialising in psoriasis, gut health and metabolic wellbeing. She offers online consultations across the UK through her Psoriasis Root Cause Programme — a structured, personalised approach to psoriasis that begins where the condition often does: inside.
Find out more about working with Kirsty by booking a free 20-minute Explore Call
References:
Castañeda-Mogollón, D., et al. (2025) https://pmc.ncbi.nlm.nih.gov/articles/PMC12029981/
Qian, Y., et al. (2024) https://pmc.ncbi.nlm.nih.gov/articles/PMC11331342/
Costache, D.O., et al. (2024) https://pmc.ncbi.nlm.nih.gov/articles/PMC10932248/
Wei, G., Shi, Z., Wu, X. and Hwang, S.T. (2023) https://pmc.ncbi.nlm.nih.gov/articles/PMC11361517/
Nguyen, N.T., et al. (2020) https://pmc.ncbi.nlm.nih.gov/articles/PMC6862295/
Furumatsu, K., et al. (2014) https://pmc.ncbi.nlm.nih.gov/articles/PMC4067745/
Hao, Y., et al. (2022) https://pmc.ncbi.nlm.nih.gov/articles/PMC9048827/